A 91-YEAR-old retired dairy farmer from North Wales is back on his tractor and enjoying five mile hikes after undergoing pioneering robotic surgery.
Great-grandfather Owen John Thomas, from Holyhead, Anglesey, was one of the first patients to have a knee replaced using the ROSA® Knee (RObotic Surgical Assistant) system at the private Spire Murrayfield hospital, Wirral, carried out by consultant hip and knee surgeon Mr Muthu Ganapathi.
The hospital is the first in the Wirral and Liverpool area to offer cutting-edge robotic technology which helps surgeons plan and perform personalised bone cuts so they can fit implants more precisely according to a patient’s individual anatomy rather than following universal surgical measurements.
The technique has been credited with achieving faster recovery times, less pain and a more ‘natural’ feel in the knee joint – with patients typically back on their feet within days.
Mr Thomas’ son, Tudor, described the surgery as “miraculous” and said his dad was on his feet – walking unaided – less than 24 hours after the operation and was already back enjoying the simple life on his tractor.
“It was miraculous how well he actually felt afterwards,” said the 66-year-old, from Holyhead, who used to work at the Wylfa nuclear power station.
“He was back on his feet straight away and hardly took any painkillers at all.
“He’s back doing what he was doing 10 or 20 years ago – it was absolutely marvellous and has definitely given him a new quality of life.”
ROSA® was initially developed for brain surgery and has been adapted for use in knee replacement procedures because it offers more precision than the human eye. Importantly, it assists the surgeon’s work with data and guidance and does not conduct the surgery itself.
The technology uses data about a patient’s knee to provide the surgeon with detailed information about their individual anatomy to enable them to plan and perform more personalised bone cuts than traditional knee replacement surgery.
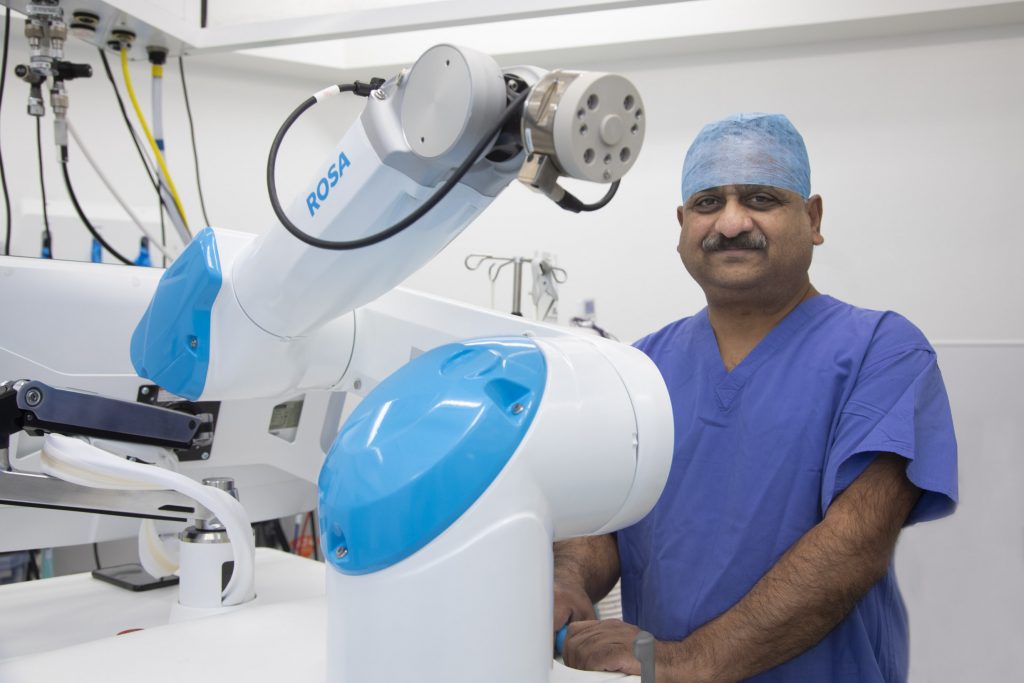
During the procedure, the technology works similar to a high-tech GPS system, mapping reference points on the knee joint from a 3D digital plan which has been fed into the ROSA system.
A camera and sensor provide live feedback to the surgeon via a digital display and, with the aid of a robotic guiding arm, the technology helps the surgeon to do precise bone cuts to place the implants according to their plan.
One of the huge advantages of the personalised Robotic assisted technique compared to traditional knee replacements is there is little to no need for soft tissue release which limits bleeding and significantly reduces post-operative pain.
Mr Ganapathi explained that while traditional knee replacements are considered a successful form of surgery, multiple studies have shown that only 80 percent of patients report optimal outcome post-surgery compared to 95 per cent of hip replacement patients.
This is probably due to traditional surgical techniques being based on universal targets of mechanical alignment which may not suit the anatomy of individual patients.
“Robotic-assisted technology has been around for more than a decade but previously it was quite cumbersome,” explained Mr Ganapathi, who lives with his family in Colwyn Bay.
“The important development now is that it allows for personalised knee replacement. Essentially, the aim of personalised alignment knee replacement is to return the knee joint close to pre-arthritic anatomy in the hope that we can reduce the proportion of dissatisfied patients.
“To use a very simple analogy, it’s the difference between wearing a ready-made shirt or wearing a shirt that has been stitched personally for you.
“To achieve this personalisation, you need a very precise tool that doesn’t rely on the human eye. That’s where the robot comes in. Medical studies have shown that the robot is more accurate than manual instruments and we can cut to within a degree or even a millimeter.

“Also, because we restore the knee to as close to how it was before, the need to do soft tissue release to make space for the implant is less. This means less pain and a faster recovery.”
Mr Thomas, who has been a widower for 15 years following the death of his wife, Mair, sought Mr Ganapathi’s expertise last year after suffering a fall and losing all mobility.
“He must’ve been suffering with arthritis in both knees for a long time,” explained Tudor.
“He couldn’t put any weight on the left knee yet he’d always been very active all his life. Previous to the fall, he was busy doing everything around the farm, driving around on his tractor.
“I was with my dad when Mr Ganapathi explained the procedure. He told us he’d already been using the method in his NHS work in North Wales and had found it very successful, so we said yes we’d go for it.”
Even though he was well-acquainted with the benefits of robot-assisted knee surgery, Mr Ganapathi was still surprised at the speed of the farmer’s recovery, given that he was 90 when he underwent the procedure.
“John was able to walk unaided with 24 hours – normally it takes around six weeks with traditional surgery,” he said.
“It’s faster recovery and less pain. Some patients are going home walking unaided within 24 hours.”
Mr Ganapathi, 56, who completed his higher specialist orthopedic training in Wales before doing further advanced training in Montreal, Canada, had already performed more than 50 robotic assisted knee replacements using in North Wales before bringing the pioneering technology to Spire Murrayfield last year.
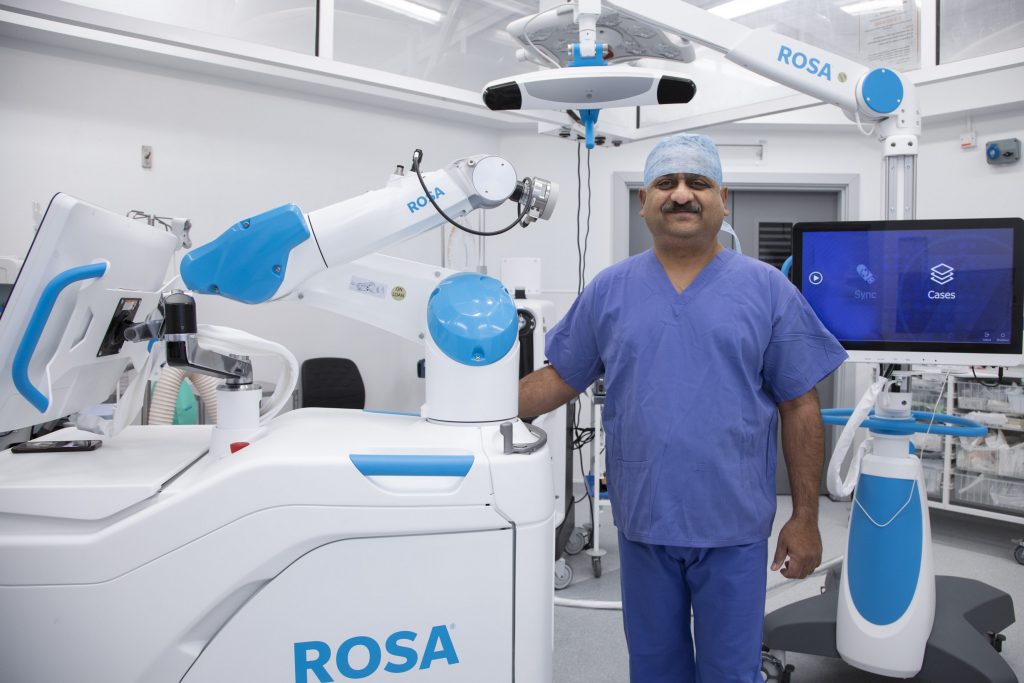
“I am glad that I am now able to offer this cutting-edge technology to my private patients as well”, he said.
He is regarded as a leading expert in the field and helps train other surgeons across the UK to perform robot-assisted knee surgery.
Mr Ganapathi was already a trailblazer having been carrying out knee replacements using MRI-based 3D moulds of the patient’s knee to achieve personalised outcomes since 2012. Robotic-assisted surgery represents a further advancement of the technique, allowing real-time planning and adjustments during the surgery itself.
“The advantage for me is I’ve been using 3D planning with 3D mould technique for many years. I have done close to a thousand 3D planned knee replacements, so I’m quite used to the approach,” he said.
“But with the robotic system you can do everything in real time. You can see the damage from arthritis and plan accordingly, even during surgery itself.”
Now fully healed, Mr Thomas is back to enjoying his regular walks and riding his tractor.
“He’s very sociable and he goes out walking to meet people and talk to people,” said Tudor, who has two grown-up sons.
“He’ll still get on his tractor, it doesn’t faze him at all, and he’s very active despite just turning 91. He will go for a walk for three, four or five miles. He’s still driving now and doing most activities.
“The difference in him now is marvellous and it’s still carried on. From my father’s experience, it’s been brilliant.”
Sean Crooks, Hospital Director at Spire Murrayfield Hospital, said: “We are thrilled to be working with this exciting technology here and improving our patients’ quality of life.”


















